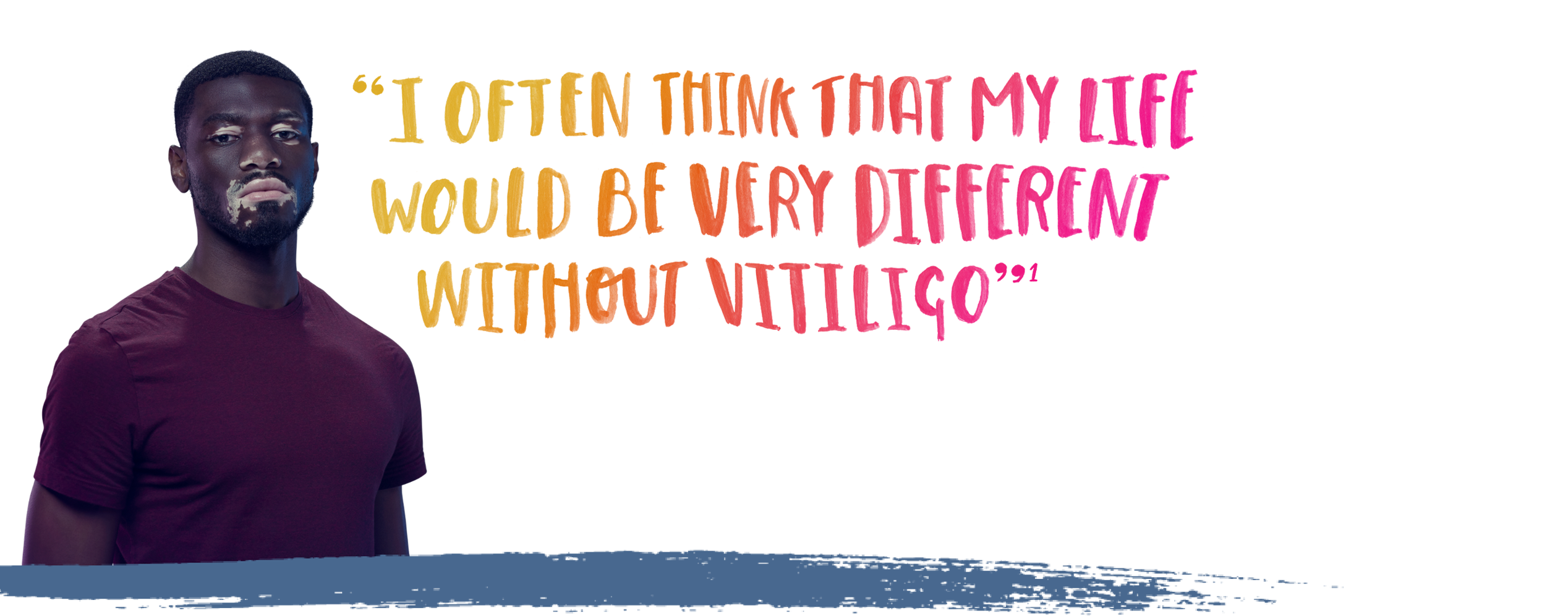A complex autoimmune disease
Vitiligo can appear anywhere on the body. It’s a disease that has a complex pathogenesis, caused by the progressive autoimmune destruction of melanocytes.1,2 This results in a condition that takes away more than just pigment, but also confidence and even career prospects — approximately 1 in 2 patients said their vitiligo impacted their career choice.1,2
Differences in skin biology3,6
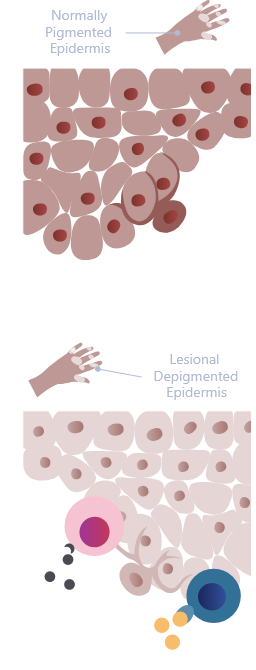
Top image adapted with permission from John Wiley & Sons, Inc. Gan EY, et al. Pigment Cell Melanoma
Res. 2017;30(1):28-40. Copyright© 2017
Bottom image adapted with permission from Frisoli ML, et al. Annu Rev Immunol. 2020;38:621-648. Copyright© 2020
Autoimmune destruction of melanocytes leads to skin depigmentation3,6
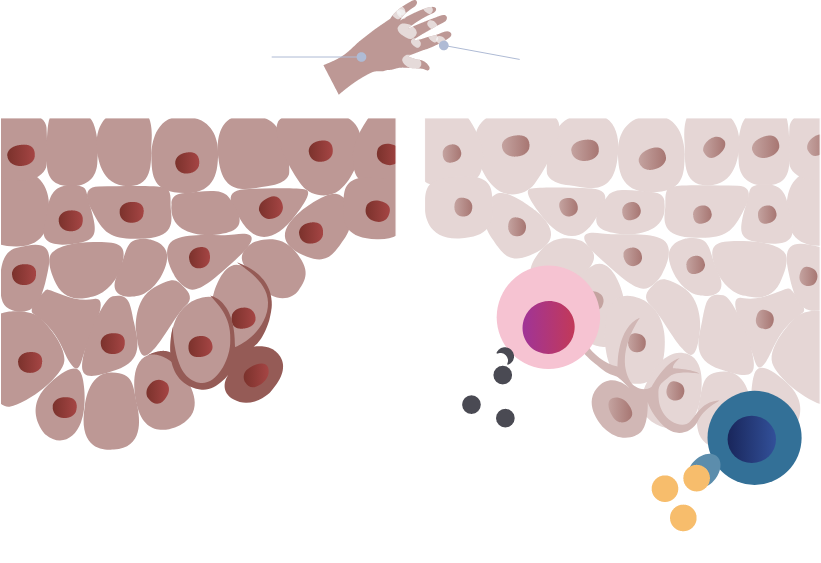
Left image adapted with permission from John Wiley & Sons, Inc. Gan EY, et al. Pigment Cell Melanoma
Res. 2017;30(1):28-40. Copyright© 2017
Right image adapted with permission from Frisoli ML, et al. Annu Rev Immunol. 2020;38:621-648. Copyright© 2020
Top image adapted with permission from John Wiley & Sons, Inc. Gan EY, et al. Pigment Cell Melanoma
Res. 2017;30(1):28-40. Copyright© 2017
Bottom image adapted with permission from Frisoli ML, et al. Annu Rev Immunol. 2020;38:621-648. Copyright© 2020
Autoimmune destruction of melanocytes leads to skin depigmentation3,6
Vitiligo is still one of the most difficult challenges in dermatology.4
What causes vitiligo?
The causes of vitiligo remain mystifying to patients. This is an issue you may find especially challenging in younger patients as they may draw their own conclusions from a lack of information. Approximately 1 in 4 patients discovers they have vitiligo before they are 10 years old, almost half of patients with vitiligo develop the disease before the age of 20 years and, for nearly 8 out of 10 patients, they discover their vitiligo before the age of 30 years.4

Adapted from Shankar. Changing faces (2022)
The many causes of vitiligo
Vitiligo is a disease caused by a dynamic interplay between several factors.8 These include:
Dysregulated immune response
- Abnormally heightened innate immunity in the skin and antibodies against melanocytes were found in patients with vitiligo4
- Immune dysfunction due to the recruitment of innate and adaptive immune cells and production of proinflammatory proteins and cytokines3
Environmental stress
- Exposure to chemicals and ultraviolet radiation3,4
- Mechanical stress, which may cause detachment and loss of melanocytes from the epidermis (melanocytorrhagy) and associated Koebner phenomenon9
- Emotional stress triggered by major life events10
Genetics
- Multiple common variants identified in innate and adaptive immune genes3
- Higher prevalence of vitiligo among patients’ immediate relatives3
- There is a 6% risk of vitiligo in a patient’s sibling8
- There is a 23% risk for identical twins8
Adapted from Kirpal's story. (2020)
Adapted from Kirpal's story. (2020)
For some patients, vitiligo is also associated with long periods of disease stability followed by shorter periods of accelerated depigmentation.12 That makes it hard for you or your patients to ever be confident that things won’t develop further. It's why approximately 3 in 4 vitiligo patients worry that their condition will get worse over time.13
What subtypes of vitiligo exist?
Varying patterns of lesional spread and progression can cause vitiligo to get misdiagnosed as other skin conditions – approximately 3 in 7 people living with vitiligo in Europe have experienced misdiagnosis.14
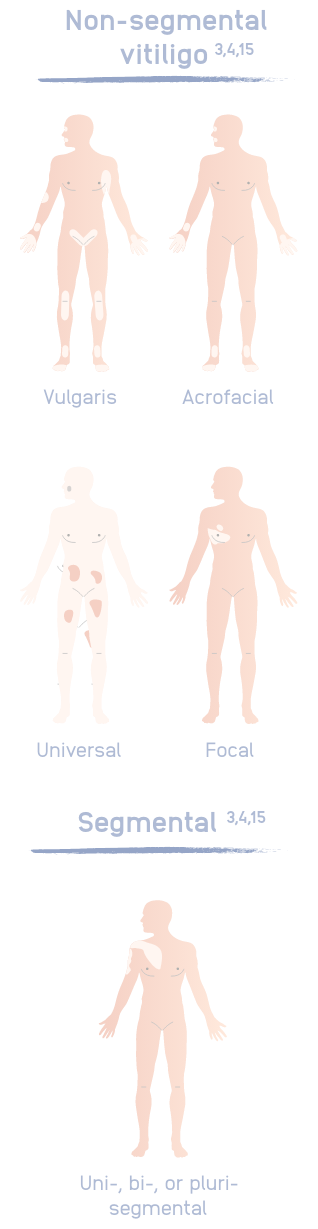
Image adapted from Picardo M, Dell’Anna ML, et al. Vitiligo. Nat Rev Dis Primer. 2015;1(1):1-16.
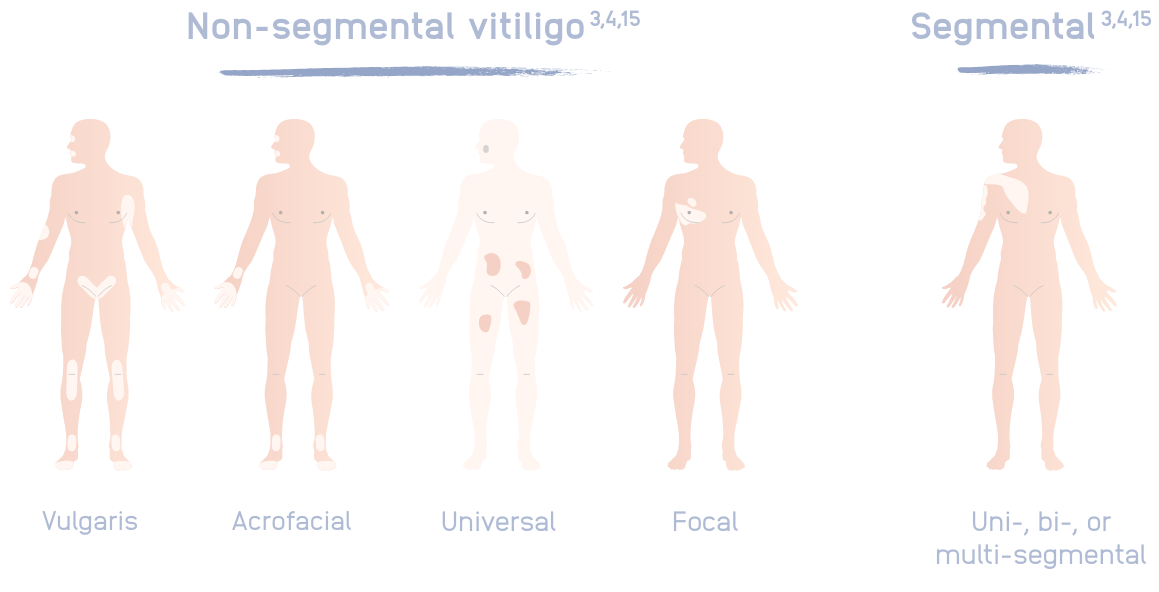
Image adapted from Picardo M, Dell’Anna ML, et al. Vitiligo. Nat Rev Dis Primer. 2015;1(1):1-16.
Non-segmental vitiligo (NSV):
- NSV presents with lesions involving both sides of the body3
- Presents towards symmetrical distribution3
- Usually progresses slowly with an unpredictable course3
- The immune system attacks functional melanocytes3,4
- Accounts for 84–95% of vitiligo cases3
Segmental vitiligo (SV):
- Usually unilateral3
- Has an earlier onset than NSV3,4
- Progresses rapidly and then stabilises3,4
- Once stabilised, SV is generally less progressive than NSV15
- Related to somatic mosaicism and not believed to have an immune aetiology3
Mixed-type vitiligo:
- Initial segmental involvement3
- Eventual onset of bilaterality3
- Usually more refractory to treatment3
It is important to clinically differentiate between NSV and SV as SV is thought to have distinct underlying pathogenetic mechanisms and shows poor response to conventional treatments. Updated and clear guidance on diagnosis is therefore key to ensure proper treatment.3,4
- Bibeau K, Hamzavi I, et al. Mental Health and Psychosocial Burden Among Patients Living With Vitiligo: Findings From the Global VALIANT Study. Presented at: Maui Derm for Dermatologists; January 24, 2022; Grand Wailea, Maui, HI.
- Ezzedine K, Eleftheriadou V, et al. Vitiligo. Lancet. 2015;386(9988):74-84.
- Picardo M, Dell’Anna ML, et al. Vitiligo. Nat Rev Dis Primer. 2015;1(1):1-16.
- Bergqvist C, Ezzedine K. Vitiligo: A Review. Dermatol Basel Switz. 2020;236(6):571-592.
- Rodrigues M, Ezzedine K, et al. New Discoveries in the Pathogenesis and Classification of Vitiligo. J Am Acad Dermatol. 2017;77(1):1-13.
- Riding RL, Harris JE. The Role of Memory CD8+ T Cells in Human Vitiligo. J Immunol. 2019;203(1):11-19.
- Shankar. Changing faces. Shankar’s story. Published online 2019. https://www.changingfaces.org.uk/story/shankars-story-it-takes-time-to-embrace-who-you-are/ #:~:text=When%20I%20was%20a%20teenager,to%20spiral%20out%20of%20control. Accessed September 2022.
- Rashighi M, Harris JE. Vitiligo Pathogenesis and Emerging Treatments. Dermatol Clin. 2017;35(2):257-265.
- Kumar R, Parsad D. Melanocytorrhagy and Apoptosis in Vitiligo: Connecting Jigsaw Pieces. Indian J Dermatol 2012.78(1):19-23.
- Papadopoulos L, Bor R, et al. Impact of Life Events on the Onset of Vitiligo in Adults: Preliminary Evidence for a Psychological Dimension in Aetiology. Clin Exp Dermatol. 1998;23(6):243-248.
- Kirpal’s story: What makes you different makes you beautiful. Published Winter 2020.
https://www.changingfaces.org.uk/story/kirpals-story-what-makes-you-different-makes-you-beautiful/. Accessed September 2022. - Gawkrodger DJ, Ormerod AD, et al. Guideline for the Diagnosis and Management of Vitiligo.
Br J Dermatol. 2008;159(5):1051-1076. - Bae JM, Lee SC, et al. Factors Affecting Quality of Life in Patients With Vitiligo: A Nationwide Study. Br J Dermatol. 2018;178(1):238-244.
- Bibeau K, Harris J, et al. Diagnosis and Management of Vitiligo From the Perspectives
of Patients and Healthcare Professionals: Findings From the Global VALIANT Study. Presented at: Maui Dermfor Dermatologists; January 24, 2022; Grand Wailea, Maui, HI. - Ezzedine K, Lim HW, et al. Revised Classification/Nomenclature of Vitiligo and Related Issues:
The Vitiligo Global Issues Consensus Conference. Pigment Cell Melanoma Res. 2012;25(3):E1-13.